Key Takeaways
- CMS virtual direct supervision rules, which became permanent on January 1, 2026, prevent contrast exam cancellations by allowing radiologists to supervise procedures remotely via real-time audio-video technology.
- Imaging facilities can mitigate cancellations caused by staffing shortages, multi-site coverage demands, and emergency backup requirements through the implementation of virtual oversight solutions.
- Virtual supervision allows a single radiologist to oversee multiple imaging sites simultaneously, reducing scheduling gaps and improving equipment utilization across a network.
- Regulatory compliance requires technology and documentation standards to meet strict CMS criteria for audio-visual connectivity and quality assurance tracking.
The permanent adoption of virtual direct supervision by the Centers for Medicare & Medicaid Services (CMS) continues to change how contrast imaging operations function. For imaging facilities struggling with consistent exam cancellations, these rules support reliable scheduling and broader patient access to diagnostic services.
2026 Regulations And The Causes of Cancellations
The 2026 Medicare Physician Fee Schedule and Hospital Outpatient Prospective Payment System Final Rules established virtual direct supervision as a permanent provision for Level 2 diagnostic tests. This category includes contrast-enhanced CT and MRI exams. This regulatory update addresses a primary cause of contrast exam cancellations: the logistical requirement for physical physician presence.
Before these updates, imaging centers often faced operational disruptions when on-site radiologist coverage was interrupted by illness, emergency calls, or conflicting schedules. The traditional mandate for physical presence meant that contrast exams were frequently postponed or canceled, creating barriers to patient care. Understanding the specific CMS definitions regarding immediate availability is essential for administrators transitioning to these new workflow models.
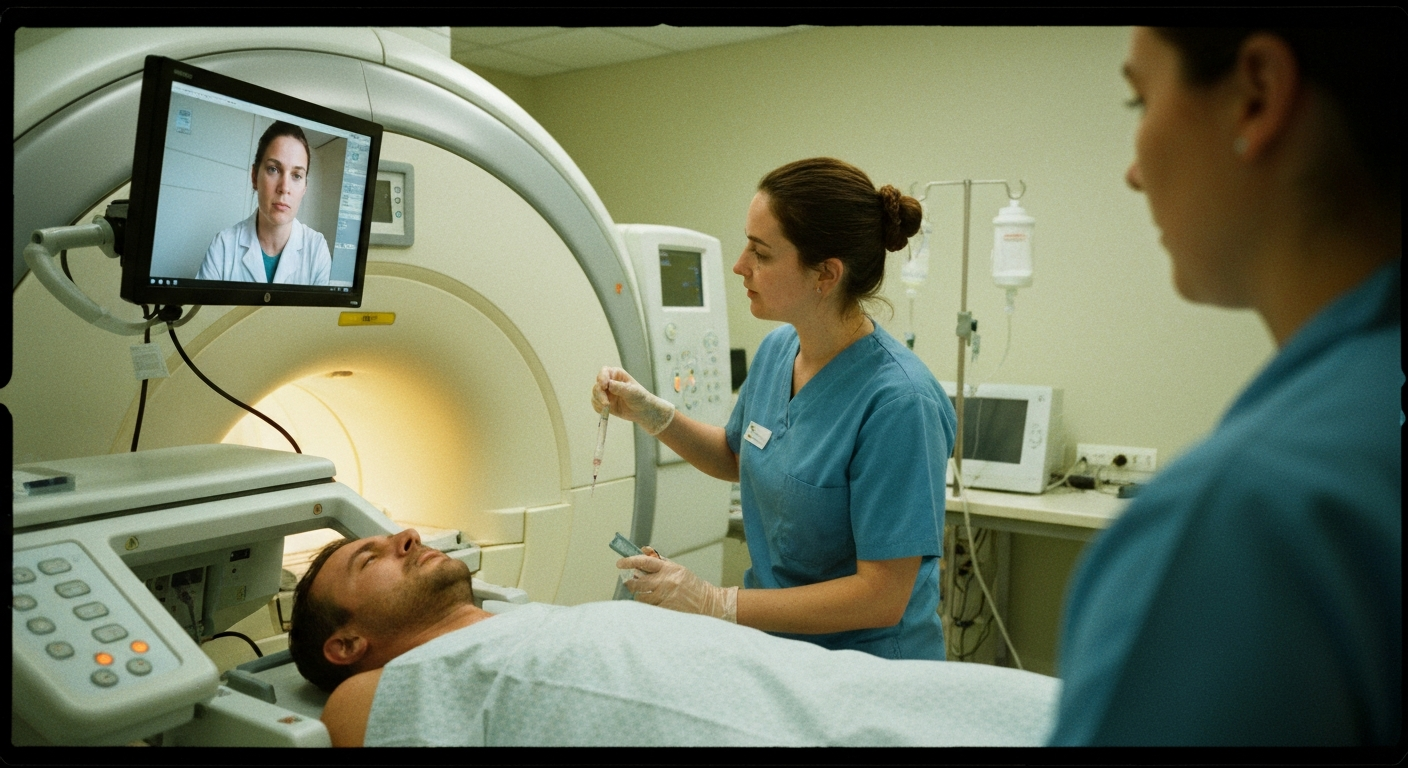
The permanent rules reduce this vulnerability by allowing specialized radiologists to provide direct supervision through real-time, two-way audio and video technology. This shift enables imaging centers to maintain continuous coverage even during unexpected staffing gaps, ensuring that scheduled contrast procedures proceed without the need for rescheduling.
Addressing Specific Causes of Cancellations
1. Staffing Gap Solutions
Radiologist shortages continue to impact imaging facilities, particularly in rural and underserved areas. Virtual supervision allows imaging centers to access a network of specialized radiologists who provide immediate oversight regardless of their physical location. When local physicians are unavailable due to planned leave, professional development, or emergencies, virtual coverage ensures that imaging schedules remain functional.
This staffing flexibility is critical during peak demand periods or when multiple radiologists are unavailable simultaneously. Rather than turning patients away, imaging centers can maintain full operational capacity through the use of established virtual supervision networks.
2. Multi-Site Coverage Optimization
Health systems operating multiple imaging locations often struggle to provide consistent on-site supervision at every facility. Virtual supervision allows a single expert radiologist to oversee contrast procedures at multiple sites from a central location. This optimizes the workforce and ensures that each facility remains compliant with supervision requirements.
This approach minimizes the logistical challenges of coordinating physician travel and reduces the risk of coverage gaps at satellite locations. Multi-site operators can design coverage models that provide reliable supervision across an entire network without requiring redundant on-site staffing at every facility.
3. Emergency Backup Protocols
Virtual supervision provides a backup system for situations that historically necessitated exam cancellations. If a scheduled on-site radiologist becomes unavailable due to an emergency, the facility can connect with backup supervisors through a virtual platform. These protocols ensure that patient care continues without the cascading schedule disruptions that occur when physical supervision is lost.
Operational Impact on Facility Workflows
Scheduling Reliability Improvements
Virtual supervision improves scheduling reliability by decoupling physician availability from physical location. Facilities can schedule contrast-enhanced studies throughout operating hours with the assurance that specialized supervision is available. This leads to higher patient satisfaction, as fewer appointments require rescheduling. Patients can depend on their appointments proceeding as planned, which facilitates faster diagnostic results and treatment planning.
Equipment Utilization and Financial Efficiency
Reliable scheduling leads to improved equipment utilization rates. MRI and CT scanners involve significant capital investment, and maximizing their use is necessary for facility financial performance. When supervision constraints no longer limit scheduling, imaging centers can operate equipment at optimal capacity. The reduction in cancellations also minimizes equipment downtime and allows for more efficient staffing of technologists and support personnel.
State Law and Regulatory Reconciliation
While CMS has established federal baseline requirements for virtual supervision, imaging facilities must remain compliant with state laws governing the scope of practice for radiologic technologists. State regulations vary regarding remote supervision; while many states align with federal CMS standards, others maintain more specific requirements for contrast administration.
Facilities should conduct regular reviews of state-specific practice acts and guidance from state medical boards. Some jurisdictions may require specific training or competency demonstrations for technologists operating under virtual supervision models. The interaction between federal CMS requirements and state law creates a compliance framework that requires careful navigation, particularly for organizations operating across multiple state lines. Ensuring that virtual supervision workflows align with these varying legal standards is a prerequisite for long-term operational success.
Technology and Documentation Standards
1. Audio-Visual Requirements
CMS mandates real-time, two-way audio and video communication for virtual direct supervision. The technology must provide immediate connectivity, allowing the supervising radiologist to observe the procedure and communicate with on-site staff. Audio-only communication is insufficient. High-definition video quality and HIPAA-compliant transmission protocols are necessary to maintain the standard of care. Technology systems must also include redundancy to prevent supervision interruptions in the event of a local network failure.
2. Documentation Protocols
Thorough documentation is required for audit readiness. Each contrast procedure must record the identity of the supervising radiologist, the method of supervision (virtual), the specific times of availability, and any clinical guidance provided. Documentation systems should generate time-stamped logs confirming that the required audio-video connectivity remained active throughout the duration of the procedure. These records serve as an audit trail for CMS reviews and internal compliance monitoring.
3. Quality Assurance and Safety Tracking
Quality assurance programs must monitor the effectiveness of virtual supervision. This includes tracking response times, technical system reliability, and patient safety outcomes. Monitoring contrast reaction management and protocol adherence ensures that virtual oversight maintains the same safety standards as traditional on-site supervision. Regular reviews of these metrics help facilities identify areas for workflow optimization and staff training.
Reducing Cancellations Through Virtual Solutions
Facilities that have integrated virtual supervision technology report measurable reductions in contrast exam cancellations. These improvements are tied directly to the increased flexibility in radiologist coverage and the ability to bridge staffing gaps in real-time. The decrease in cancellations correlates with increased procedure volumes, better equipment utilization, and improved patient retention.
Beyond the financial and operational benefits, reducing cancellations facilitates more timely medical decision-making. Patients receive critical diagnostic imaging without the delays associated with supervision-related rescheduling. For imaging center administrators, the transition to virtual oversight represents a method for ensuring CMS compliance while stabilizing daily operations in an increasingly difficult staffing environment.
Note: Information provided is for general guidance only and does not constitute medical, legal, or financial advice. Pricing estimates and regulatory requirements are current at the time of writing and subject to change. For personalized consultation on imaging center operations and virtual contrast supervision, contact ContrastConnect.
ContrastConnect
Las vegas
Las Vegas
NV
89109
United States

